Managed Care Digest Series® Spotlight
Lines of Business Shift in 2020 for Commercial Insurers
Commercial insurers reported strong earnings in 2020—record levels in many cases—despite a 3.2% annual
drop in employer-sponsored insurance membership.1,2
Elevated earnings were attributable to two factors:
1) pandemic-induced deferral of care; and 2) penetration
into public insurance programs. The drop in medical
utilization in 2020 likely led to the first time—since at
least 1960—that U.S. health expenditures decreased
annually, while the diversification of business lines reflects
a years-long strategy for many insurers (see also page 6).3
With earnings strong and interest rates low, large
commercial insurers are either deleveraging from
previous acquisitions, as in the case of
CVS Health,
or investing further through strategic acquisitions.4
The rise of telemedicine is driving both technology
investments and plan redesigns. For example, virtual-first
plans are meant to capitalize on recent changes
in consumer and provider preferences, while also
delivering on promises to reduce health care inflation.
To enhance its digital strategy, UnitedHealth Group
purchased Change Healthcare, a health analytics
and technology company.5 And in particularly frank
remarks soon before announcing the purchase of
MDLIVE, the CEO of Cigna described sustainability
problems that health care systems face globally.6
Assets tied to public health insurance programs also
remain attractive, especially given recent enrollment
trends.7 In June 2021, Anthem acquired managed
Medicare and Medicaid plans in Puerto Rico from
MMM Holdings.8 Later that year, GuideWell, the parent
company of Florida Blue, announced a similar acquisition
of Puerto Rico-based Triple-S Management.9 Centene,
one of the largest offerors of managed care for public
programs, acquired a technology company, Apixio;
a specialty pharmacy, PANTHERx; and a diversified
behavioral health company, Magellan Health. Centene
announced a major restructuring initiative soon after.10
Finally, to address rising costs and expand its use of
value-based care, Humana completed the purchase of
Kindred at Home in August 2021, instantly becoming the
nation’s largest provider of care in the home.11 Given the
recent struggles of residential long-term care facilities
and the relative success of hospital-at-home programs,
it would not be surprising to see more insurers focus
increasingly on the home as a primary site of care.
Click here to read the 2021 Commercial Payer Digest ™.
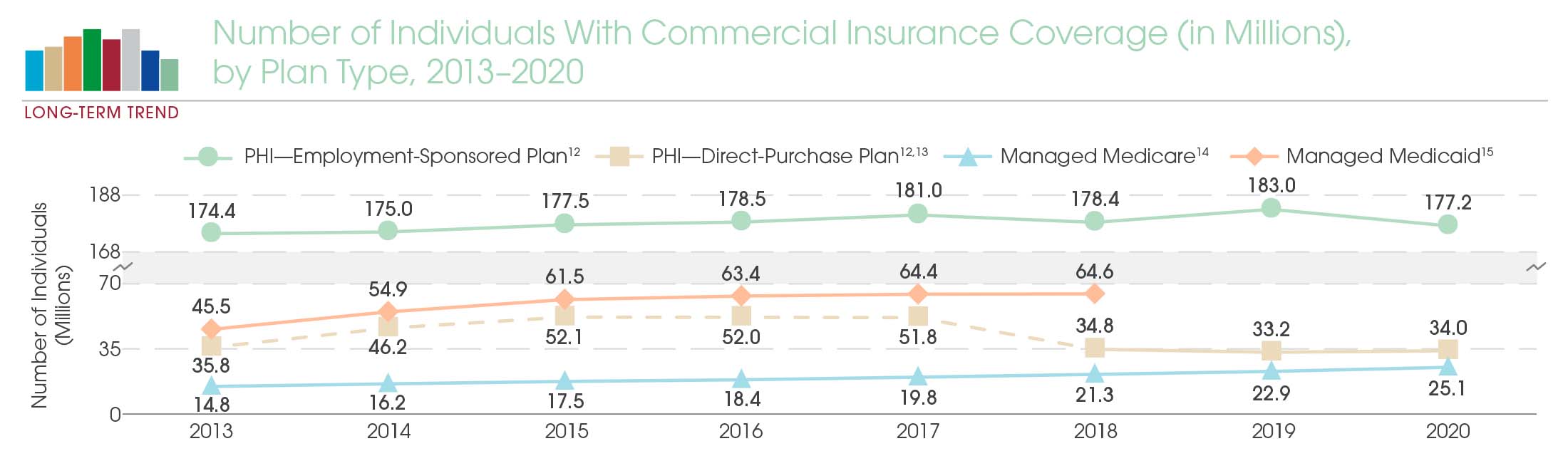
Data sources: U.S. Census Bureau and Centers for Medicare & Medicaid Services © 2021
NOTE: Throughout this digest, PHI is private health insurance.
Read More Articles >>